- Like
- SHARE
- Digg
- Del
- Tumblr
- VKontakte
- Flattr
- Buffer
- Love This
- Save
- Odnoklassniki
- Meneame
- Blogger
- Amazon
- Yahoo Mail
- Gmail
- AOL
- Newsvine
- HackerNews
- Evernote
- MySpace
- Mail.ru
- Viadeo
- Line
- Comments
- Yummly
- SMS
- Viber
- Telegram
- JOIN
- Skype
- Facebook Messenger
- Kakao
- LiveJournal
- Yammer
- Edgar
- Fintel
- Mix
- Instapaper
- Copy Link
 Fat Isn’t Making You Fat
Fat Isn’t Making You Fat
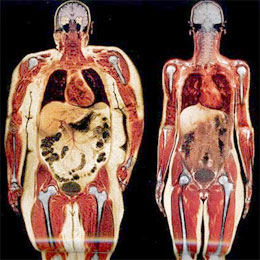
It should not be particularly surprising that foods high in fat are consumed every day. From deep fried butter to bacon wrapped meatloaf, where does all of the fat go?
Physical measures such as expanding waistline, bulging stomach, etc. are easy to see, but what about people that never seem to gain weight?
The less obvious consequences of fat overdose may be more problematic in the long run.
It’s What’s Inside That Matters Most: Subcutaneous Fat vs. Visceral Fat
Subcutaneous Fat
 Subcutaneous fat is the fat that is visibly present in overweight people. It is found just beneath the skin and is the area that you pinch when you need motivation to exercise. Subcutaneous fat acts as a cushion that absorbs shock in event the body is subject to trauma. It also stores energy that the body uses during periods of high energy consumption. Of course, too much of a good thing can be bad. Added weight due to overeating and lack of physical activity increases the amount of stress placed on joints and can increase the risk of heart disease. Although subcutaneous fat may not be attractive, it is not as harmful to the body as visceral fat. Removal of subcutaneous fat in obese women through liposuction had no effect on blood sugar, blood pressure, or cholesterol levels three months after the operation.1
Subcutaneous fat is the fat that is visibly present in overweight people. It is found just beneath the skin and is the area that you pinch when you need motivation to exercise. Subcutaneous fat acts as a cushion that absorbs shock in event the body is subject to trauma. It also stores energy that the body uses during periods of high energy consumption. Of course, too much of a good thing can be bad. Added weight due to overeating and lack of physical activity increases the amount of stress placed on joints and can increase the risk of heart disease. Although subcutaneous fat may not be attractive, it is not as harmful to the body as visceral fat. Removal of subcutaneous fat in obese women through liposuction had no effect on blood sugar, blood pressure, or cholesterol levels three months after the operation.1
People that continuously eat fatty or sugary foods, but never seem to get fat may be harboring more fat that you think. If you’ve ever heard the term skinny-fat or thin outside, fat inside, you know that there are many people who look healthy on the outside, but may have large amounts of fat surrounding their internal organs. This type of fat is called visceral fat and it’s important to know the difference.
Visceral Fat
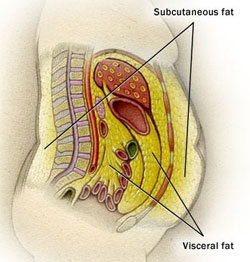 Visceral fat is body fat typically stored within your body around the abdominal cavity, which is where vital organs, such as the liver, pancreas, and intestines, reside. Visceral fat is metabolically active. What this means is that visceral fat generates bioactive molecules that can have detrimental effects on the body. When visceral fat is metabolized by the liver, it is transformed into cholesterol. Cholesterol circulates throughout the blood and may eventually collect in arteries, increasing the chance of heart disease and high blood pressure.2
Visceral fat is body fat typically stored within your body around the abdominal cavity, which is where vital organs, such as the liver, pancreas, and intestines, reside. Visceral fat is metabolically active. What this means is that visceral fat generates bioactive molecules that can have detrimental effects on the body. When visceral fat is metabolized by the liver, it is transformed into cholesterol. Cholesterol circulates throughout the blood and may eventually collect in arteries, increasing the chance of heart disease and high blood pressure.2
In case you were wondering how people maintain their physique while gaining visceral adiposity, the answer lies within exercise—or rather lack thereof, and diet. Fat will accumulate inside the body if the body is not moving. Without movement, there is no means to metabolize the fat. What makes the situation worse is if a large quantity of foods high in saturated fat (butter, cheese, cakes, etc) are being consumed because almost all of this fat is stored as visceral fat.
What is non-alcoholic fatty liver disease or NAFLD?
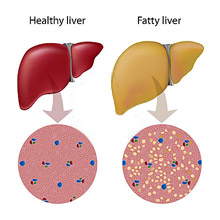 Non-alcoholic fatty liver disease (NAFLD) is exactly as the name describes: the accumulation of fat in the liver of people that drink little to no alcohol.
Non-alcoholic fatty liver disease (NAFLD) is exactly as the name describes: the accumulation of fat in the liver of people that drink little to no alcohol.
NAFLD is very common and the majority of patients exhibit few or no symptoms; however, if the disease progresses, excess fat from elevated blood lipids such as cholesterol and triglycerides will be deposited in the liver as a function of insulin resistance and the metabolic syndrome characterized by diabetes. This can cause inflammation and scarring of liver tissue and may result in liver failure.3
How does fat consumption affect NAFLD?
- Total fat intake: Increased fat intake may result in subsequent insulin resistance and impaired lipid metabolism. Consumption of excess energy through fatty foods will result in a large amount of free fatty acids in the circulation. High free fatty acid levels in plasma will eventually lead to fat accumulation in other organs such as the liver (NAFLD) or skeletal muscles. Free fatty acids are detrimental to health because of their ability to accumulate in peripheral organs, but mainly the liver in NAFLD. Free fatty acids are prominent in NAFLD and therefore reduction of total fat intake is advised.4
- Saturated fat: Saturated fatty acids have been shown to have adverse effects on NAFLD as they increase total cholesterol levels, but more specifically LDL levels. Saturated fatty acid intake should be less than 7% of total fats and energy intake in all individuals, but those diagnosed with NAFLD in particular.5
- Monounsaturated fatty acid (MUFA): MUFAs have positive effects on cardiovascular function and have the ability to decrease oxidized low-density lipoprotein cholesterol levels decreasing blood cholesterol levels.4 They also function as a means to transport fat soluble vitamins and minerals. Therefore individuals diagnosed with NAFLD should increase consumption of MUFAs to incur these benefits.
- Polyunsaturated fatty acid (PUFA): Polyunsaturated fatty acids (PUFAs) contain both n-3 and n-6 fatty acids. The ratio of n-6/n-3 fatty acids is important as some studies showed that consumption of both of these fatty acid compounds had potential benefits for NAFLD patients. In vitro studies in both animal models and human intervention studies showed beneficial effects of n-3 PUFAs as a treatment of NAFLD in humans as well as CHD.6,7 Both MUFAs and PUFAs have been known to reduce the adverse effects of type 2 diabetes. This is important because type 2 diabetes can potentially lead to NAFLD.
What healthy foods are high in monounsaturated fat (MUFA)?
 Popular MUFA foods:
Popular MUFA foods:
- Nuts
- Vegetable oils
- Canola oil
- Olive oil
- High oleic safflower oil
- Sunflower oil
- Avocado
What healthy foods are high in polyunsaturated fat (PUFA)?
 Popular PUFA foods:
Popular PUFA foods:
- Soybean oil
- Corn oil
- Safflower oil
- Canola oil
- Walnuts
- Flaxseed
- Fish (trout, herring, mackerel, and salmon)
How does weight loss affect NAFLD?
As the number of cases of obesity increases, there is a subsequent increase in prevalence of NAFLD.8 Patients with NAFLD have been shown to have higher energy intake in comparison to healthy controls. This means that the majority of the fat in the liver has been accumulated from diet and consumption alone. This would suggest that in order to reduce the risks associated with NAFLD, gradual weight loss should be implemented in obese or overweight patients. Weight loss can improve metabolic parameters and subsequent liver histology i.e. inflammation by reducing fat buildup as well as releasing proteins and enzymes that could otherwise trigger the inflammatory response.8
Diets low in either carbohydrates or fatty acids will serve to promote long term weight loss; constant and strict diet monitoring is advised.4 A combination of increased physical activity and diet modification is the most effective therapy for NAFLD. Even slight weight loss can be beneficial and could “reverse” the disease to some extent.
Is NAFLD associated with other chronic diseases?
Excessive fat in the bloodstream/circulation of fat in the plasma will cause fat to accumulate in improper places. Free fatty acids can directly affect beta cells in the pancreas and therefore affect insulin production or resistance.9 The cells will become less responsive to blood sugar and resistant to insulin due to the large amount of free fatty acids in the bloodstream. Resistance to insulin will eventually lead to type two diabetes mellitus.
This increased risk of diabetes will most likely cause a confluent increase in the risk of cardiovascular disease (although these factors do not develop independently). Individuals with an impaired glucose tolerance may exhibit other comorbidities such as hypertension or macroangiopathy which would then cause an increase in the risk for cardiovascular disease. However, in independent studies, data showed that NAFLD is associated with a twofold greater risk of developing cardiovascular disease than those without; however, there are no conclusive studies that can adequately indicate cause and effect.10
Should I go on a no-fat or low-fat diet?
When researchers looked at how low-fat diets could affect normal women in terms of overall health, weight gain, and cholesterol levels, it was found that low fat diets did not provide a significant difference.11 Growing children, pregnant or lactating women, and the elderly have different essential fatty acid requirements as well as caloric density, so limiting fat consumption to the point of deprivation can increase the risk of detrimental health effects.
Common Reasons to Get Liposuction
 A lot of people go to the gym and take long runs every day to stay in shape.
A lot of people go to the gym and take long runs every day to stay in shape.
But there are some people who even after putting so much hard work into their exercises just cannot get rid of that extra fat.
You can get rid of healthy fat quite easily, but the obstinate fats are the real challenge! It does not go away easily and can be very stubborn.
This is why a lot of people opt for Liposuction as it helps them get rid of that disproportionate fat and makes them look fit.
It is the most common and popular type of cosmetic surgery in the US, and the reason behind that is because it is safe and very effective. Let’s take a look at a few of the major reasons due to which people opt for liposuction.
Body Reshaping
Even if you have achieved your desired weight, you can still end up being unhappy with your body shape. This happens when you have obstinate fats in one area of your body. When you are already in your desired shape when it comes to other parts of the body, it can be hard to get rid of fats from that specific area. With the help of liposuction, you can get rid of that fat without losing any weight or going on an unhealthy diet. It can give your body the perfect proportions you have always wanted. If you are also thinking of getting a lipo treatment, then you can consult at www.breslowmd.com/liposuction/ as well.
To Boost Self Confidence
Having unwanted fat on your body even after putting in hours of hard work can really damage your confidence. You will feel like you worked for nothing, and it just demotivates you to work on yourself. This is why a lot of people opt for liposuction, so they do not have to feel bad about all the hard work they put. You already got yourself in the best shape you could; only the stubborn fat is left, which can be taken out with liposuction, so there is no need to feel bad about it.
For Staying Healthy
Sometimes the number of obstinate fats in the body can pass the normal levels, and it can become dangerous for your health. With the help of liposuction, you can get rid of triglycerides in the blood and can reduce your risks of heart diseases. Even though triglycerides are formed naturally in the body, studies have shown that they can be reduced by 40% after liposuction.
Reducing Fat Production
Another reason people opt for liposuction is that it does not only get rid of the excessive stubborn fat existing in your body already, but it reduces its production as well. The science is simple; with the help of liposuction, you are not just removing fat; you are removing fat-producing cells as well, which means it is unlikely that you will gain such huge amounts again. However, even after the removal of fat cells, you would have to work out and keep up a healthy routine in order to stay fit.
The Bottom Line
In the end, what is most important is the type of fat consumed and not the amount. Healthy fats provide the body with the feeling of satiation that can potentially contribute to weight loss. Absence of fat in the diet may result in fatigue, dry skin and hair, depression, hormone imbalances and weight problems.
As stated previously, not all fats are bad. Monounsaturated fatty acids (MUFAs) and polyunsaturated fatty acids (PUFAs) are good examples of fats necessary for normal bodily function. If you need to eat fats regardless, then it would be a good idea to consume these types of fats compared to unhealthy fat alternatives (see food list above for foods high in MUFAs and PUFAs). Of course, as with all things, a balanced diet alongside consistent exercise will go a long way.
References:
1. Klein S, Fontana L, Young L, et al. Absence of an effect of liposuction on insulin action and risk factors for coronary heart disease. The New England Journal of Medicine. 2004;350(25):2549–2557.
2. Després JP. Cardiovascular disease under the influence of excess visceral fat. Critical Pathways in Cardiology. 2007;6(2):51–59.
3. Musso G, Cassader M, Rosina F, Gambino R (2012) Impact of current treatments on liver disease, glucose metabolism and cardiovascular risk in non-alcoholic fatty liver disease (NAFLD): a systematic review and meta-analysis of randomised trials. Diabetologia 55: 885–904.
4. Rafiq, N., & Younossi, Z. (2008). Effects of weight loss on nonalcoholic fatty liver disease. Seminars in Liver Disease, 25(4), 427-433.
5. McCarthy, E. M., & Rinella, M. E. (2011). The role of diet and nutrient composition in nonalcoholic fatty liver disease. Journal of the Academy of Nutrition and Dietetics, 112(3), 401-409. doi: 10.1016/j.jada.2011.10.007.
6. Spadaro L, Magliocco O, Spampinato D, Piro S, Oliveri C, Alagona C, Papa G, Rabuazzo AM, Purrello F. Effects of n-3 polyunsaturated fatty acids in subjects with nonalcoholic fatty liver disease. Dig Liver Dis. 2008;40:194–199.
7. McCarthy, E. M., & Rinella, M. E. (2011). The role of diet and nutrient composition in nonalcoholic fatty liver disease. Journal of the Academy of Nutrition and Dietetics, 112(3), 401-409. doi: 10.1016/j.jada.2011.10.007.
8. Argo CK, Caldwell SH. Epidemiology and natural history of non-alcoholic steatohepatitis. Clin Liver Dis. 2009;13:511–531.
9. Klonoff, D., Buse, J., & Nielsen, L. (2008). Exenatide effects on diabetes, obesity, cardiovascular risk factors and hepatic biomarkers in patients with type 2 diabetes treated for at least 3 years. CMRO,24(1), 275-286.
10. Sookoian S, Pirola CJ. Non-alcoholic fatty liver disease is strongly associated with carotid atherosclerosis: A systematic review. J Hepatol. 2008;49:600–607.
11. Krauss RM, Deckelbaum RJ, Ernst N, Fisher E, Howard BV, Knopp RH, Kotchen T, Lichtenstein AH, McGill HC, Pearson TA, Prewitt TE, Stone NJ, VanHorn L, Weinberg R. Dietary guidelines for healthy American adults.Circulation. 1996;94:1795–1800.
About Joanna Lo
Joanna graduated with a B.S. in Nutrition – Biochemistry from the University of California, Davis. She has worked on research studies at several laboratories including the UCD Medical Center research building, the UCD Center for Neuroscience, and the Western Human Nutrition Research Center, one of the six USDA-funded human nutrition centers in the country.